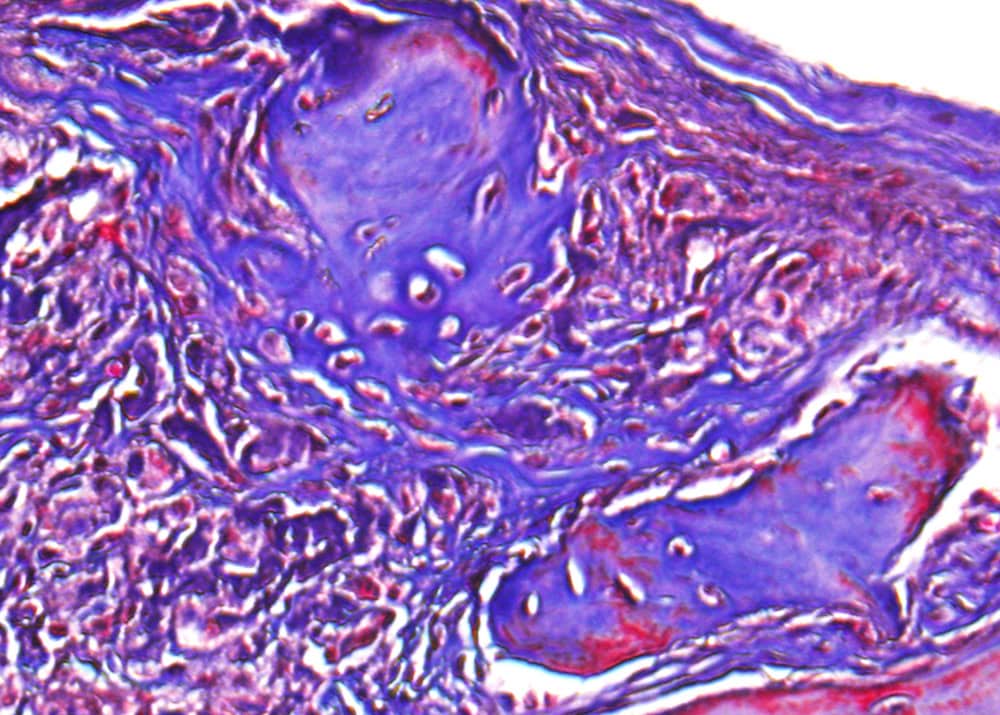
[Image above] Histological analysis of bone regeneration in mouse skull defects at 6 weeks post-surgery. Credit: University of California, Los Angeles
When I begin a large research project, I often start my search in two places: Wikipedia and Encyclopædia Britannica.
These two sites are good at providing general topic overviews, and the references act as great primary sources to provide more detailed information.
However, these sites are not infallible, which I noticed when researching the applications of clay.
If you look up clay on Wikipedia and Britannica, the pages are filled with information on clay’s applications in building and pottery/art. Yet medical applications, another important use of clay, make no appearance on Britannica and are mentioned in only three short sentences on Wikipedia’s main clay page. (Wikipedia does have a more detailed medicinal clay page, though.)
People have used clay for medical purposes, such as wound healing and hemorrhage inhibition, since ancient times. Current commercial pharmaceuticals include clays and clay minerals as active ingredients or excipients, and interactions between clay nanoparticles and drugs are being investigated for controlled drug delivery.
Researchers are also investigating clay’s potential usefulness in another medical area: tissue engineering.
Tissue engineering is a branch of regenerative medicine that focuses on replacing or regenerating tissues to restore normal biological function. Of the potential natural and synthetic materials investigated for tissue engineering, hydrogels have received significant attention.
Hydrogels are a 3D network of polymer chains that, depending on the polymer, can be bioactive. Compared to hard scaffolds that require preshaping, soft hydrogels are injectable and can fill irregularly-shaped defects in a minimally invasive manner.
However, for hydrogels to promote tissue formation, they must be suitably porous to allow cells to migrate, infiltrate, and proliferate in the 3D environment. And creating porous hydrogel is where clay comes into play.
In an open-access paper published in Nature Communications, researchers from the University of California, Los Angeles, increased the pore size in their previously-developed hydrogel made of methacrylated glycol chitosan (MeGC) by combining it with the clay montmorillonite (MMT).
MMT is a layered silicate [(Na,Ca)0.33(Al,Mg)2Si4O10(OH)2•nH2O] that shows no negative effects in studies on possible acute and chronic toxicities. It is also a major component of bentonite, which is already approved by the FDA as an additive in various medicinal products.
To create their clay-enhanced hydrogel, the researchers used intercalation chemistry to introduce nanoclay particles into the in situ-forming hydrogel. They then used a process called photoinduction to turn the biomaterial into a gel, which simplified injection into mice with nonhealing skull defects.

Alkaline phosphatase (ALP) activity in the engineered tissue. (ALP is an enzyme present in high concentrations in bone cells.) In vitro characterization of the combination of MeGC and MMT, confirmed with ALP and mineralization staining, showed the optimal weight of MMT was 1.5% weight/volume. Credit: Cui et al., Nature Communications (CC BY 4.0)
After six weeks, the researchers euthanized the mice and harvested their tissues for analysis. They discovered the tissues showed significant bone healing “only by applying the material itself in the absence of cells or growth factors.”
“This feature is of importance for translation to the clinical application, as cells were not necessary to be harvested and re-implanted back to the patients or expensive growth factors, such as BMP-2, to be applied,” they explain.
The researchers note they did not test mechanical properties of the regenerated bone because the defect was small and the healing site was not load-bearing. “[T]he further study of biomechanical properties will be needed in other fracture models such as large segmental defects,” they add.
The open-access paper, published in Nature Communications, is “Microporous methacrylated glycol chitosan-montmorillonite nanocomposite hydrogel for bone tissue engineering” (DOI: 10.1038/s41467-019-11511-3).
Update 09/13/2019 – Reworded to clarify that some, but not all, hydrogels are bioactive.
Author
Lisa McDonald
CTT Categories
- Biomaterials & Medical