[Image above] philippe leroyer; Flickr CC BY-NC-ND 2.0
The numbers say that at least 21% of you have one or more tattoos. And those odds jump to ~40% if I consider “you” to be only those readers in the 18–29-year-old range.
That’s a lot of ink.
But do you know why that ink stays put, despite constant renewal of your skin cells? A new video by the American Chemical Society’s Reactions series explains the fascinating science behind the permanency of tattoos.
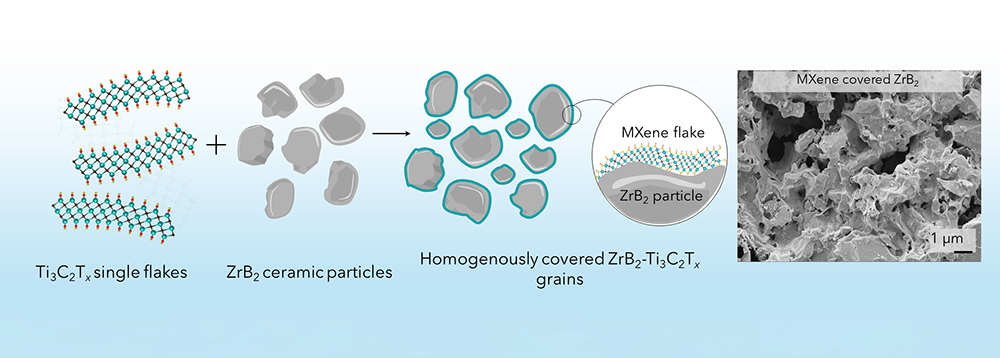
Tattoo ink consists of solid pigment particles in a liquid carrier. Different pigment compounds create different ink colors, and many of those pigment particles just happen to be ceramic materials.
Here’s the full breakdown of what common pigment compounds, many of which are metal oxides, color tattoo inks.
Those inks enter into the skin through tiny punctures wounds, created by a tattoo needle jabbing your skin at a painful 50–3,000 times per minute.
The needle punctures through the outermost layer of skin, the epithelium, and breaks into the underlying layer, the dermis. Capillary action draws the ink down into the punctures, pulling those tiny pigment particles deep down in to the dermis.
This is an important point because the skin’s outer epithelium sloughs off and replaces itself roughly every 2–3 weeks. It’s essentially a skin cell conveyer belt—new epithelial cells regenerate at the base of the epithelial layer, migrate up to the top, and eventually are sloughed off, contributing to that layer of dust accumulating on your dresser.
The dermis doesn’t go through the constant renewal cycle of the epithelium. But despite the prime skin layer locale, it’s really your immune system you have to thank—or curse—for that ink staying put.
The tattoo needle pounding away creates micro-damage to your skin, which illicits an immune response to repair the damage. Your immune system sends its best recruits to the damage to try to repair the wound and save your skin (literally).
Those recruits—macrophages—are cells that serve as the body’s garbage men, cleaning up pathogens, dead cells, and various other junk. In newly-tattooed skin, macrophages do their job, gobbling up ink particles in an attempt to clear them from the wound.
But that’s as far as the hungry macrophages get—with bellies full of ink, they get stuck in the dermis. Although the macrophages eventually die, they get swallowed up by new, yet equally stuck, macrophages, making the tattoo visible for the rest of your life. (The ink does break down a little over time, but largely it stays put.)
So next time you go get a tattoo—perhaps one ode to science—be sure to thank ceramics.

Credit: Reactions; Youtube
UPDATE (August 7, 2015):
CTT reader Bart Kilinski pointed out that several of the substances listed in the tattoo ink infographic above are indeed toxic substances—particularly cinnabar and cadmium and chrome oxides. “Surely those aren’t used in tattooing,” Kilinski comments.
Well, Bart—it’s true. Many toxic substances were historically used in tattooing, and several still are.
It’s important to note that, perhaps surprisingly, the FDA does not regulate tattoo inks. Tattoo parlors are regulated, but “because of other public health priorities and a previous lack of evidence of safety concerns, the FDA has not traditionally regulated tattoo inks or the pigments used in them,” the agency states on its website.
At the First International Conference on Tattoo Safety, held in Berlin in June 2013, researchers at the National Institute of Health in Rome, Italy—among many others—presented their scientific research on tattoo safety. Their abstract, titled “Heavy metals in tattoo inks,” states, “Titanium, barium, aluminum, and copper are often used as colorants in tattoos; more worrisome, inks using nonmetal colorants may include traces of antimony, arsenic, cadmium, chromium, cobalt, lead, and nickel.”
According to a Scientific American article, red tattoo inks cause the most problems. The heavy metals in red inks and other ink colors can cause allergic reactions, skin conditions, scarring, and mercury sensitivity.
Those problems seem to be relatively rare, although I couldn’t find any statistics pinpointing the exact number. General allergic reactions to tattoos, not necessarily attributed to metal-containing inks, are themselves relatively infrequent.
A rather informal poll by NBC News in New York City earlier this year put that number at 4% of inked people experiencing a short-duration allergic reaction and 6% experiencing problems lasting more than four months. But those problems can be attributed to a range of issues, including individuals’ immune systems, other compounds in tattoo inks, and problems with hygiene or practice in specific tattoo parlors.
In addition to skin-related problems, metal-containing tattoo inks can also—even more rarely—cause burns during an MRI.
But I want to go back to the problems with red ink, though, which our reader Bart so observantly noted.
University College London researcher and preserved tattoo expert Gemma Angel confirms that cinnabar was used in early 20th century tattoos. Cinnabar is an ore of mercury, so its not surprising that Angel also reports that many 20th century medical journal articles that refer to cinnabar tattoo ink are describing cases of toxicity.
In 1930, one such case appeared in the Archives of Dermatology and Syphilology, written by Dr. Paul Gerson Unna. His patient, a 63-year-old man who had been tattooed in his youth, suddenly developed itching, swelling and blistering in the red portions of the tattoo, following a mercury-based treatment for hemorrhoids. Three years later, Dr. D. B. Ballin reported a case in which a young male patient had developed itching, swelling and oozing in the red portions of a tattoo, 2 years after he had been tattooed. The patient was treated by the removal of the affected areas using a dermal punch, and the tattooed skin samples were sent for histological testing; however, the resultant scar tissue in the punched areas later developed the same reaction.
From what I can find, cinnabar isn’t used in tattoo inks today. However, cinnabar is still an ingredient in several Chinese medicines, although studies have found that the mercurial compound has “relatively low toxic potential when taken orally.”
In fact, many heavy metals are actually essential for life, and only become toxic at higher exposures. So I suppose it’s true: The only difference between medicine and poison is in the dose.
One problem and source of confusion regarding heavy metal toxicity goes back to how to experimentally evaluate how the compounds in tattoo ink impact human health.
According to an article published in Environmental Health Perspectives:
Understanding exposure to lead and other metals once incorporated into a tattoo is not simple. A healed tattoo is a complicated array of ink particles trapped within dermal fibroblasts, macrophages, and mast cells. ‘One of the biggest problems is, over the period of time, how is exposure evaluated?’ says Westley Wood, president of Unimax Supply, a tattoo equipment supplier and ink producer, which settled out of court in the AESI lawsuit. ‘Should it be counted every single day for the rest of your life, or is it dissipated in the body within a month?’
Although ink alternatives exist, however, simply getting inked with heavy metal-free pigments won’t solve all your problems, according to the American Academy of Dermatology:
The composition of tattoo ink has changed dramatically over the years. In the past, metal salts, lead, cobalt, and carbon were used in inks. Today, many modern tattoo inks (especially intense reds and yellows) contain organic azo dyes with plastic-based pigments that also have industrial uses in printing, textiles, and car paint. As a result, Dr. Shinohara explained that there are many unknowns about how these inks interact with the skin and within the body and if they are responsible for an increasing number of complications.
Those complications also include allergic reactions, infections, and bumps.
So, Bart, I hope that answers your question. Toxic particles are used or have been used in tattoo inks, although those substances don’t necessarily (but can!) cause toxicity. This may be due to their residence contained within macrophages, which shield the body from further exposure to the compound—or it could be due to some other completely different reason. Only more science will tell.
Author
April Gocha
CTT Categories
- Art & Archaeology
- Material Innovations
- Nanomaterials