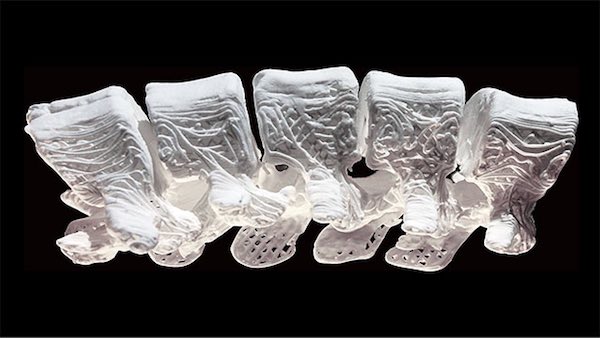
[Image above] Hyperelastic bone 3-D-printed in the shape of a section of the human spine. Credit: Adam E. Jakus
Whether you’re attacked by a bear (twice) or trip and fall because you’re distracted by a set of see-through bathrooms, at some point most of us need help repairing these impressive bodies we live in.
So an important goal of biomaterials research is to be able to repair and replace bone when and where we need it. And although much success has been made in this area—such as here, here, here, here, here, or here—we still don’t have an ideal biomaterial with widespread clinical availability.
That ideal material needs to be robust enough to match the strength of natural bone, yet flexible enough to integrate with the body—and biocompatible, rapidly deployable (even in the operating room), customizable, and reasonably scalable. Oh, and how about an inexpensive price tag, too?
While that may sound like a lofty wish list, researchers at Northwestern University report that they’ve developed a hyperelastic material that can be 3-D-printed into a potential bone replacement scaffold that ticks all those boxes.
The material is a 3-D printable ink that consists of hydroxyapatite and a biodegradable, biocompatible polymer binder [the team tested two different biocompatible polymers, polycaprolactone and poly(lactic-co-glycolic acid), that are already used in medicine and tissue engineering applications] in a solvent that evaporates during printing. The liquid ink can be rapidly 3-D-printed at room temperature.
The key to the new material is its Goldilocks combination of materials to provide strength and flexibility.
Hydroxyapatite, a natural component of bone and teeth, has long been explored as a bone replacement material. But hydroxyapatite alone is hard and brittle. Mixing hydroxyapatite with polymers can help afford flexibility, but too much polymer can inhibit the bioceramic’s activity.
Which is why the Northwestern scientists’ ratio is just right—their unique mixture of 90% hydroxyapatite and 10% polymer is strong enough to serve as a bone replacement, but flexible enough to be easily integrated and adapted into the body.
But in addition to adequate material properties, a bone replacement material must also have an ideal structure.
“Porosity is huge when it comes to tissue regeneration, because you want cells and blood vessels to infiltrate the scaffold,” Ramille Shah, assistant professor of materials science and engineering at Northwestern and lead researcher on the new study, says in a Northwestern news story. “Our 3-D structure has different levels of porosity that is advantageous for its physical and biological properties.”
Watch this short Science video to see how the new porous material can bend without breaking.

Credit: Science Magazine; YouTube
As a material, the new hyperelastic bone passes all the material properties necessary to stand up with bone, too. According to the new paper’s abstract, “The resulting 3-D-printed hyperelastic bone exhibited elastic mechanical properties (~32 to 67% strain to failure, ~4 to 11 MPa elastic modulus), was highly absorbent (50% material porosity), supported cell viability and proliferation, and induced osteogenic differentiation of bone marrow–derived human mesenchymal stem cells cultured in vitro over 4 weeks without any osteo-inducing factors in the medium.”
The Northwestern team tested the hyperelastic bone in mouse, rat, and primate models, which all showed promising results. However, there is a lot more work to be done before the materials can make their way into humans. According to an article on The Verge, Shah says she hopes human trials can happen within five years.
In the animal tests, however, the 3-D printed hyperelastic bone material integrated well with surrounding tissues and showed excellent biocompatibility. Stem cells infiltrated the scaffolds, vascularized the area, and even laid down new bone into the scaffolds in a short time period—all without added biological factors, which are often necessary with synthetic bone replacement materials.
But, because the 3-D printing process is done at room temperature, that possibility also exists. “We can incorporate antibiotics to reduce the possibility of infection after surgery,” Shah says in the Northwestern news story. “We also can combine the ink with different types of growth factors, if needed, to further enhance regeneration. It’s really a multi-functional material.”
The new hydroxyapatite–polymer ink requires no drying time or post-processing after printing, opening the possibility of directly integrating such 3-D printers into hospitals. Doctors and surgeons could 3-D print bone replacement materials as needed, offering the possibility of personalized solutions to repair our unique skeletal needs.
The open-access paper, published in Science Translational Medicine, is “Hyperelastic ‘bone’: A highly versatile, growth factor–free, osteoregenerative, scalable, and surgically friendly biomaterial” (DOI: 10.1126/scitranslmed.aaf7704).
Author
April Gocha
CTT Categories
- Biomaterials & Medical
- Manufacturing
- Material Innovations


